Introduction
Diabetes and gum health share a silent, two-way relationship that many people discover far too late. In the UK alone, ONS estimates over 4.3 million people live with diabetes, and clinical dental data shows they face a significantly higher risk of gum disease than non-diabetics. What’s often missed is that gum problems don’t just result from diabetes — they can actively worsen blood sugar control. Just as UK education and population bodies like ONS, HESA, UCAS, UKCISA, and QS rely on data-driven risk assessment, modern dentistry now treats oral health as a measurable systemic factor. Understanding this link isn’t optional — it’s preventative healthcare.
1. Why Diabetes Makes Gums More Vulnerable Than You Realise

Many people manage diabetes carefully yet still struggle with unexpected gum problems. The reason lies in how elevated blood glucose weakens immune defence and restricts blood flow to the gums. Research consistently shows that people with diabetes are up to three times more likely to develop severe periodontal disease.
Clinical studies highlight that high glucose levels increase inflammatory responses in gum tissue, accelerating breakdown even when brushing habits seem “normal.” In real-world terms, this means gum damage progresses faster and heals slower.
When blood sugar is well controlled, outcomes improve dramatically. Evidence suggests that maintaining stable glucose levels could reduce periodontal progression by around 35–40%. For patients, this isn’t about perfection — it’s about reducing unnecessary risk through awareness and early care.
2. How Gum Disease Quietly Disrupts Blood Sugar Control
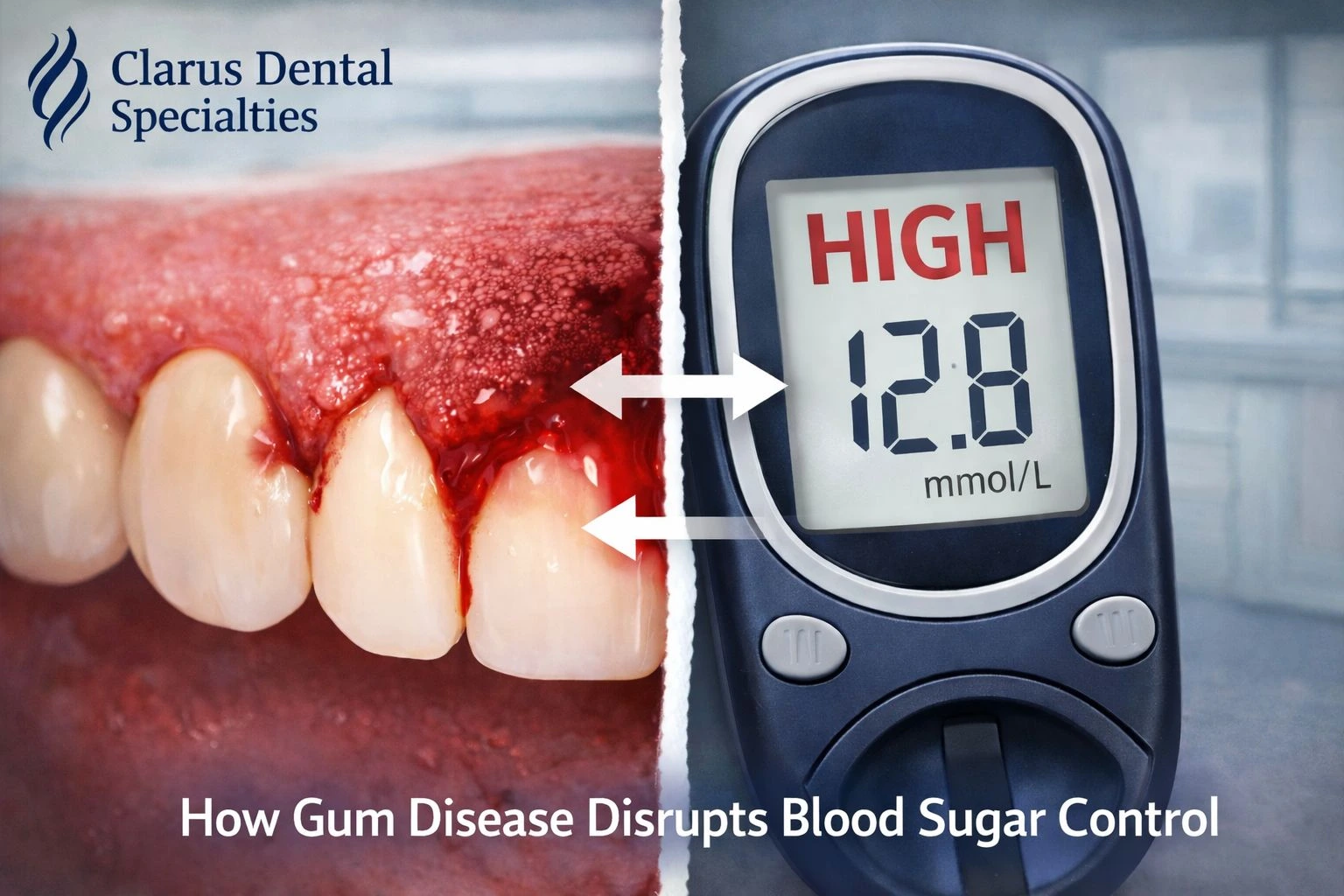
What surprises many patients is that the damage doesn’t stop at the mouth. Chronic gum inflammation releases inflammatory chemicals into the bloodstream, directly interfering with insulin sensitivity.
Multiple clinical reviews show that untreated gum disease can increase HbA1c levels by approximately 0.4–0.6%, which is clinically significant for diabetes management. In contrast, patients who receive periodontal treatment often see improved glucose control within three to six months.
This supports a growing hypothesis in medical-dental research: effective gum treatment may enhance insulin efficiency by up to 20%. In practical terms, gum care can act as a supportive therapy alongside medication, diet, and exercise — not a replacement, but a powerful addition.
3. Early Gum Symptoms Diabetics Commonly Ignore (But Shouldn’t)

Bleeding gums are often dismissed as “normal brushing issues.” For people with diabetes, they are not. Alongside persistent bad breath, gum swelling, or receding gums, these are early warning signs of a process that escalates quickly.
Surveys indicate that nearly half of diabetic adults delay treatment until gum disease reaches an advanced stage. By then, intervention becomes more complex and costly.
Research shows that early periodontal treatment can reduce the need for surgical procedures by over 50%. Acting at the first sign of trouble may also reduce long-term dental and medical complications by around 45% — a meaningful difference driven purely by timing.
4. Why Your Dentist Plays a Bigger Role Than You Think

The modern dentist is no longer focused only on teeth. Periodontal screening is increasingly recognised as part of overall health monitoring, especially for high-risk patients.
Studies show that professional gum care can reduce systemic inflammatory markers in diabetic patients by up to 30%. Integrated care models — where dentists and physicians communicate — consistently report better patient outcomes.
The emerging view is clear: collaboration between medical and dental care may improve diabetes control by approximately 25% over time. This makes regular dental visits a proactive health decision, not a cosmetic one.
5. What Daily Oral Care Looks Like for People with Diabetes

Good oral hygiene isn’t complicated — but consistency matters more for diabetics than for anyone else. Brushing twice daily, cleaning between teeth, and attending professional cleanings can significantly slow gum disease progression.
Data shows that proper daily oral care reduces periodontal risk by up to 40%, while more frequent professional cleanings (every 3–6 months) are linked to far better long-term gum stability in diabetic patients.
Preventive strategies may reduce the incidence of severe gum disease by as much as 50%, offering one of the highest return-on-effort habits in diabetes management.
6. The Long-Term Cost of Ignoring Gum Health
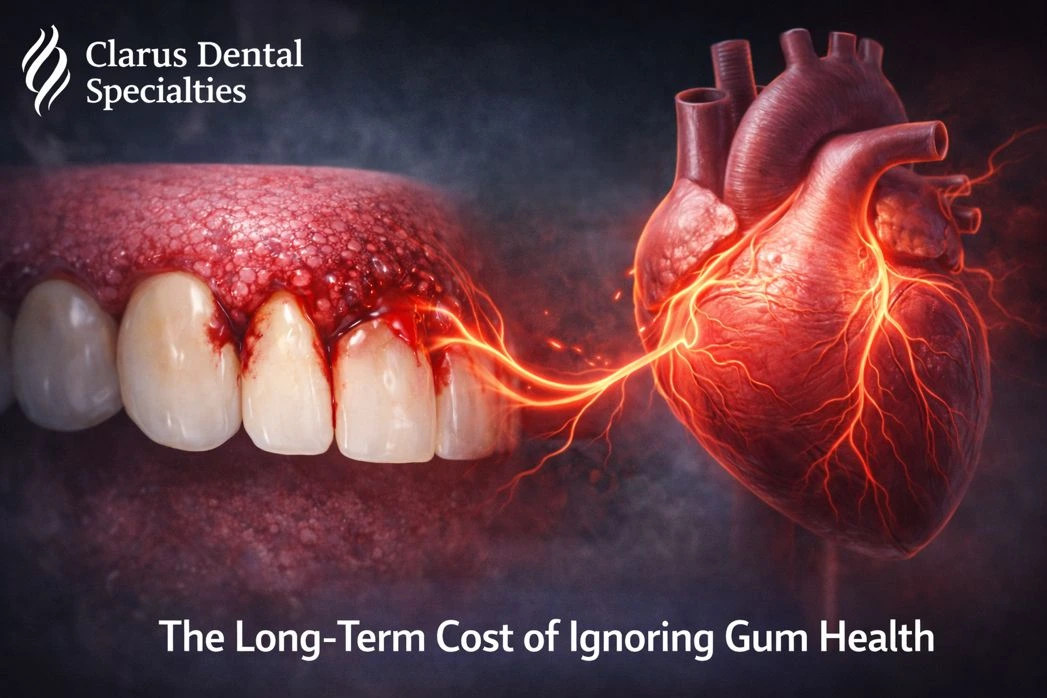
Ignoring gum health doesn’t just mean losing teeth. Advanced periodontal disease increases systemic inflammation and has been linked to cardiovascular complications.
Research indicates that diabetics with severe gum disease are twice as likely to experience cardiovascular issues compared to those with healthy gums. Long-term observational studies also associate poor oral health with higher hospitalisation rates.
The long-term hypothesis is compelling: maintaining gum health could lower diabetes-related complications by around 30% over ten years, significantly improving quality of life and reducing healthcare burden.
If you have diabetes and notice bleeding gums, swelling, or persistent oral discomfort, a preventive dental consultation can help detect issues early. Clinics like Clarus Dental focus on comprehensive gum care tailored for diabetic patients.
Comparison: Diabetes Outcomes With vs Without Gum Care
Area
- Gum Disease Progression
- Blood Sugar Stability
- Tooth Retention
- Inflammation Levels
- Long-Term Healthcare Costs
With Regular Gum Care
- Slow, manageable
- Improved
- High
- Lower
- Reduced
Without Gum Care
- Rapid, severe
- Unstable
- Increased tooth loss
- Chronically elevated
- Significantly higher
Frequently Asked Questions
1. Can diabetes directly cause gum disease?
Diabetes doesn’t directly cause gum disease, but elevated blood sugar weakens immunity and healing, making infections more likely and more severe.
2. Does treating gum disease really help blood sugar control?
Yes. Studies consistently show modest but clinically meaningful improvements in HbA1c after periodontal treatment.
3. How often should diabetics see a dentist?
Most benefit from visits every 3–6 months, depending on gum health and diabetes stability.
4. Are bleeding gums normal if you have diabetes?
No. Bleeding gums are an early warning sign and should always be evaluated.
5. Can gum disease be reversed in diabetics?
Early-stage gum disease is reversible with professional care and good daily hygiene.
